We are extremely excited that this month the paper by Jin et al. Automated detection of focal cortical dysplasia type II with surface-based magnetic resonance imaging postprocessing and machine learning was published in Epilepsia.
We are extremely excited that this month the paper by Jin et al. Automated detection of focal cortical dysplasia type II with surface-based magnetic resonance imaging postprocessing and machine learning was published in Epilepsia.
In early 2017, shortly after we published a single-centre study on automated lesion detection in children, Dr Balu Krishnan and Dr Irene Wang from the Cleveland Clinic contacted Konrad Wagstyl and myself saying that they wanted to try out our lesion detection method on a cohort of their patients. All the code was freely available and we were delighted that other centres were interested in the method and in testing it. We wanted to know if the method was robust and reproducible. Would it work on an independent cohort? Would it work on cohorts scanned on a mix of different MRI scanners? Would it work if 3D FLAIR data was not available? Would it be able to detect MRI-negative lesions?
The cohort included in the paper had included 61 patients with drug-resistant epilepsy from 3 different epilepsy centers scanned using 3 different MRI scanners. All patients had histopathologically confirmed FCD type II. MRI features were calculated off the volumetric 3T T1-weighted data. These were used to train a neural network to differentiate lesional from non-lesional cortex. The classifier outputs a probability map where values closer to 1 are more likely to be lesional and values closer to zero are more likely to be healthy cortex. The threshold of this output probability map was optimised by performing receiver operating characteristic (ROC) analyses.
The trained neural network was able to detect 73% of lesions with a specificity of 90%! ![]()
Here are some examples of the lesions it was able to detect:
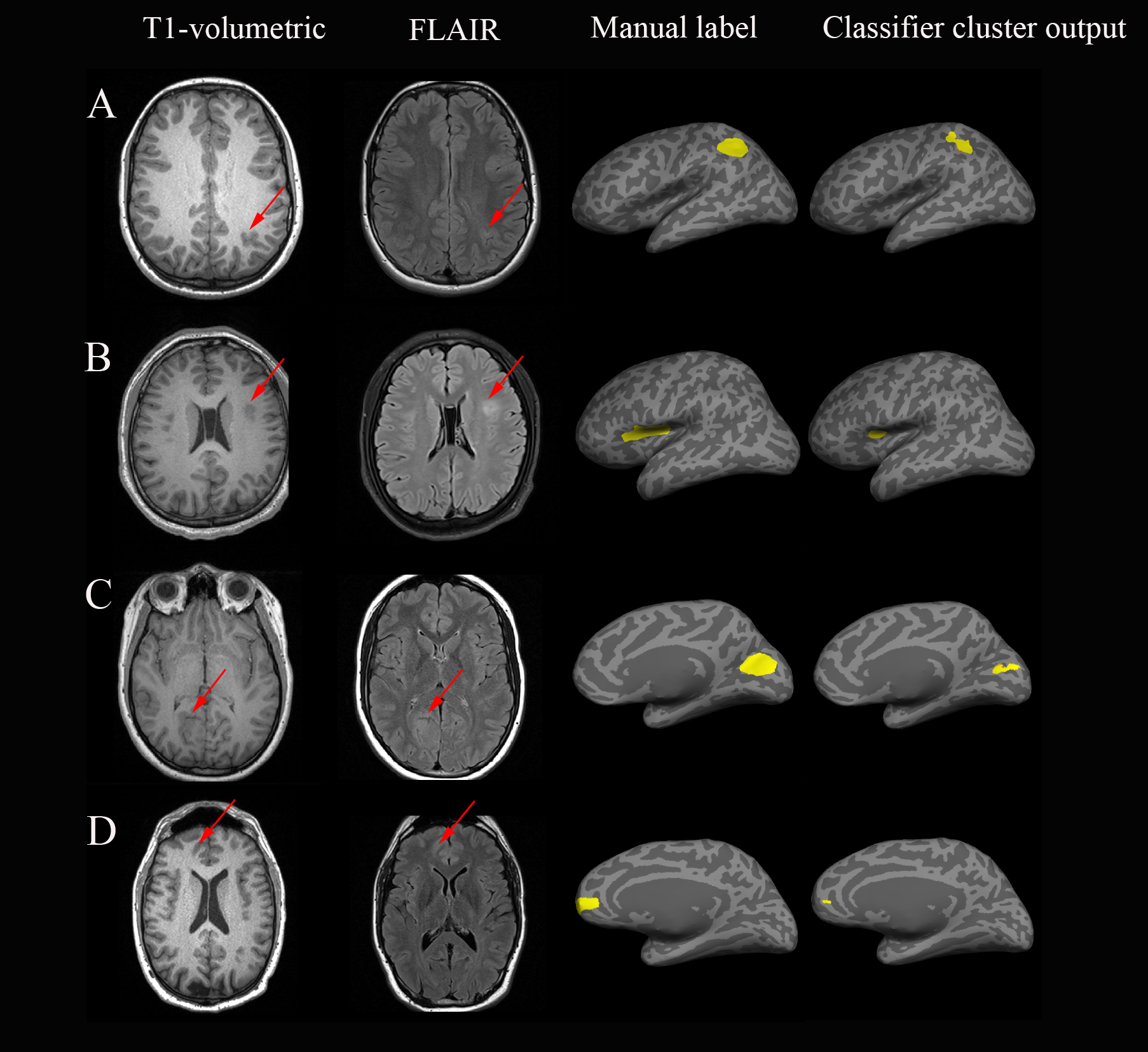
A few really exciting findings from the paper:
- out of the 17 patients with initially normal MRI scans, the machine learning method was still able to detect 53% of these lesions!!
- melding data from 3 different sites improves classifier performance over training from smaller cohorts scanned at one site.
- the number of patients used to train the classifier had a large impact on the sensitivity of the classifier - this allowed us to work out the ideal number of patients we would need to optimise the classifier (~350)!
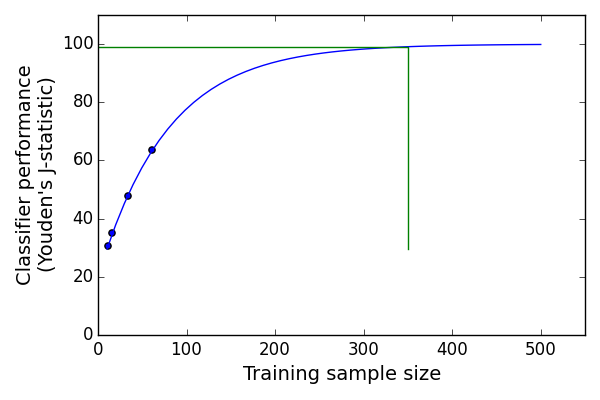
This paper reinforces that automated surface-based MRI morphometry equipped with machine learning can effectively detect subtle focal cortical dysplasias and may be a valuable tool to improve FCD detection in the presurgical evaluation of patients with pharmacoresistant epilepsy. The method was able to work on independent cohorts scanned on different MRI scanners. It was able to work on data where 3D FLAIR was unavailable AND it was able to detect lesions in a proportion of patients who are thought to be MRI-negative on visual inspection ![]() .
.
It provides renewed momentum for our MELD study. Through international collaboration and a multi-centre effort, we hope to be able to:
- train multiple epilepsy centres on the pre-processing required for surface-based MRI morphometry and machine learning
- increase understanding of the morphological characteristics of FCDs
- train an optimal neural network that can be disseminated later for multiple centres to use
- create clinically useful, open-access tools to assist in the pre-surgical evaluation of patients with drug-resistant epilepsy
It is still not too late to join the MELD Project - you can contact us at MELD.study@gmail.com.
Acknowledgements
THANK YOU to all the authors - it has been such a pleasure to work with you ![]()
![]()
